This is not meant to scare people, Its meant to inform, prevent, and talk about what almost no one wants to talk about!
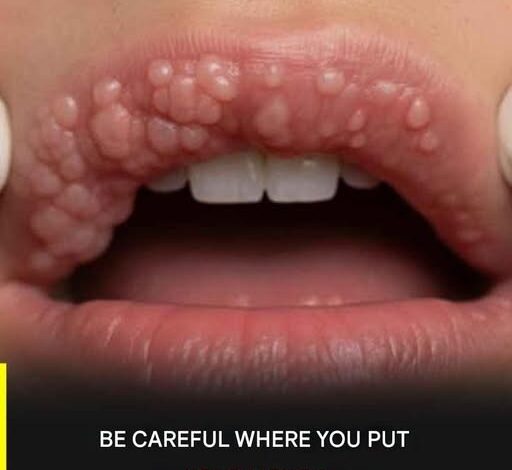
The conversation surrounding Human Papillomavirus (HPV) is often muffled by a combination of social stigma, outdated information, and a general reluctance to discuss the realities of sexual health. Yet, silence is the greatest ally of this virus. HPV is not a niche medical concern; it is the most common sexually transmitted infection on the planet. Statistical data suggests a staggering reality: four out of every five people will contract at least one strain of the virus at some point in their lives. It is a near-universal human experience, yet many remain in the dark about its classification, its link to serious illness, and the remarkably effective tools we have to neutralize its threat. This isn’t an exercise in alarmism; it is a necessary roadmap for prevention, intended to replace fear with the power of informed decision-making.
Decoding the Virus: A Spectrum of Risk
HPV is not a single entity but a diverse family of more than 100 related viruses. These viruses are specialists, evolved to affect the skin and the moist mucous membranes of the body. To manage the clinical approach to the virus, medical professionals divide these strains into two distinct categories based on their oncogenic, or cancer-causing, potential.
Low-risk HPV strains are the most common and are primarily associated with benign developments. These may manifest as genital warts or minor cellular changes that rarely, if ever, progress into something more sinister. While they can cause significant psychological distress and physical discomfort, they do not threaten the life of the host. High-risk HPV, however, is a different story. Approximately 15 strains fall into this category, and they are the primary architects of several types of cancer. While cervical cancer is the most well-known consequence, high-risk HPV is also a confirmed driver of anal, penile, vulvar, vaginal, and oropharyngeal (throat) cancers.
Dismantling the Myths
The persistence of misinformation is perhaps the greatest barrier to eradicating HPV-related diseases. To move forward, we must systematically dismantle the myths that prevent people from seeking care or vaccination.
One of the most damaging fallacies is the belief that HPV is exclusively a “woman’s problem.” While the historical focus has been on cervical cancer screening, the virus is entirely gender-neutral. Men are not only primary carriers who can transmit the virus to partners, but they also suffer from HPV-related cancers of the throat, anus, and penis. Because men do not have a routine screening equivalent to the Pap smear, their infections often go undetected until they manifest as serious illness.
Another common misconception involves the mode of transmission. In an attempt to distance themselves from the stigma of an STI, some suggest that HPV can be contracted from toilet seats, swimming pools, or shared towels. The scientific reality is more direct: HPV is transmitted through skin-to-skin and mucous membrane contact, typically during vaginal, anal, or oral sex. It is a virus of intimacy, not a virus of poor hygiene. Furthermore, the absence of symptoms does not equate to the absence of infection. Most people who carry HPV are completely asymptomatic, meaning they can unknowingly pass the virus to others for years.
The Invisible Link: HPV and Cancer
The connection between HPV and cervical cancer is one of the most clearly established links in oncology. It is estimated that 99% of all cervical cancer cases are caused by high-risk HPV persistent infections. Specifically, genotypes 16 and 18 are responsible for over 70% of these cases globally. The numbers are sobering: thousands of women are diagnosed annually, and in regions with limited access to screening, it remains a leading cause of death for young women in the prime of their lives.
However, the narrative is shifting. We are no longer defenseless. By understanding that cancer is the final, avoidable stage of a long-term viral infection, we can intervene years—even decades—before a cell becomes malignant.
The Two Pillars of Prevention
Effective protection against HPV is built on a dual-layered strategy: stopping the infection before it starts (primary prevention) and catching cellular changes early (secondary prevention).
Primary prevention begins with Comprehensive Sexuality Education (CSE). By providing young people with accurate, non-judgmental information about reproductive health, we empower them to use protection and understand the risks of skin-to-skin transmission. The second, and perhaps most powerful, tool is the HPV vaccine. Modern vaccines protect against the most dangerous high-risk strains and the strains responsible for most genital warts. Integrated into national immunization schedules for children—typically around age 11—the vaccine works best when administered before a person is ever exposed to the virus. It is a literal “cancer vaccine,” a triumph of modern medicine that has the potential to make cervical cancer a disease of the past.
Secondary prevention is the safety net for those who have already been exposed. The Pap smear (or Pap test) remains a gold standard for detecting abnormal cell changes in the cervix. By identifying these “pre-cancerous” lesions, doctors can treat them with simple procedures, preventing cancer from ever developing. In recent years, the HPV test has emerged as a vital companion to the Pap smear. By testing directly for the presence of high-risk viral DNA, doctors can identify individuals who need closer monitoring, even if their cells currently look normal.
A Collective Responsibility
The eradication of HPV-related suffering requires a comprehensive, societal approach. It is not enough for the information to exist in medical journals; it must be accessible in schools, community centers, and homes. We must work to reduce the stigma associated with the virus so that a positive test result is viewed as a manageable health data point rather than a source of shame.
When we invest in vaccination and regular screening, we aren’t just protecting ourselves; we are protecting our partners and future generations. The tools at our disposal—education, vaccination, and early detection—are incredibly effective. We have the rare opportunity to virtually eliminate a form of cancer that has claimed millions of lives. Taking responsibility for our sexual health through regular checkups and informed conversations is a fundamental act of self-care and community service.
Information is the ultimate vaccine against fear. By understanding the reality of HPV, we can make decisions that safeguard our long-term health and ensure that a common virus doesn’t turn into a life-threatening tragedy. The path forward is clear: educate, vaccinate, and screen. Through these three actions, we can change the statistics and reclaim the narrative of our own health.